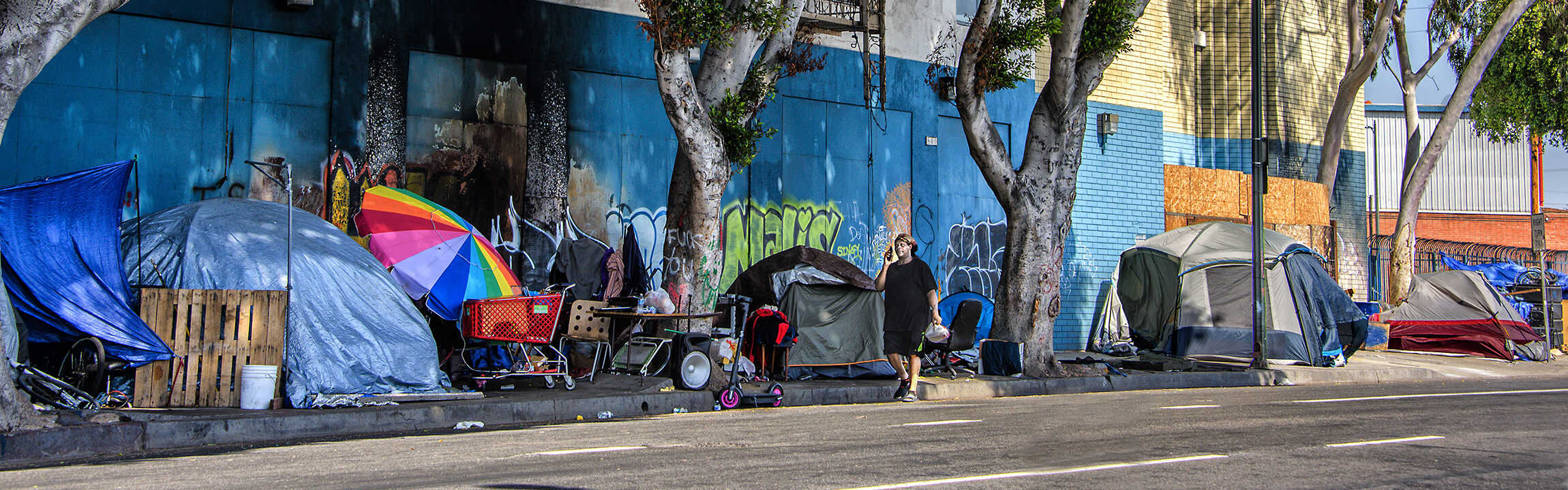When homelessness emerged in American cities during the eighties at rates similar to those seen in the Great Depression, people were shocked, and nowadays this issue is far from obsolete (Gowan 44). The relationship between mental health issues and homelessness has always been at the forefront of the concern over housing insecurity and societal perceptions of the homeless that dictate the policy that governs them. Studies have shown that about half of homeless people have traumatic brain injuries — far above the amount recorded for the general population. This, combined with the emotional trauma associated with living on the streets, is conducive to significant mental health problems that can be observed in the homeless population (Padgett). Especially in California, homelessness has become a crisis. There are about 113,000 people in California at any time who are homeless, of which 25% are considered chronically homeless (Vogel). About 70% of the homeless in California live outside a shelter compared to 5% in New York. In addition, about 25% of the homeless adults studied in Los Angeles County suffer from a severe mental illness, suggesting a strong correlation between homelessness and mental illness.
As housing prices increase and homelessness becomes more prevalent in California, addressing the mental health ailments of this population becomes increasingly important in improving their quality of life and addressing the issue of homelessness as a whole. While most welfare efforts are targeted at keeping people off of the streets, there are not enough efforts focused on eliminating the root of the problem (Streeter et. al). This study focuses on the concerns that are associated with the access of mental health resources for the homeless, the existing social welfare programs that are targeted towards mental health in the homeless population, the issues with these programs, and what can be done to solve these discrepancies. By volunteering with a program aimed at helping the homeless, I got a better understanding of the field to help evaluate what should be done to address the epidemic of mental illness in the Californian homeless population. I observed both the triumphs and shortcomings of the shelter and ultimately realized that despite its helpful philanthropic efforts, facilities like the Day House cannot be a long-term solution to the homelessness crisis in California.
To learn about resources available to the unhoused, I volunteered at the Dorothy Day House, a homeless shelter in Berkeley, California, that hosts about 30-50 residents and provides hundreds of meals every day to food-insecure people living at other shelters or on the street. While working at this facility, I was able to experience the attitudes that fellow volunteers had towards the homeless who came there for their meals and generally understand the systems that are in place to assist the unhoused who may or may not suffer from mental illness. I was also able to observe the effects of mental illness on some of the people whom the shelter served. Overall, this experience provided deep insight — in the forms of conversations with shelter volunteers and residents as well as observation of the operations in the establishment — into the inner workings of organizations and welfare programs targeted at helping the homeless.
When I initially arrived at the shelter, it was a Saturday for the dinner shift. My job was to help prep meals as a kitchen assistant. The volunteer coordinator, Eve, was an elderly lady who was warm and kind to all the volunteers, and any time a shelter resident asked her for peanut butter, or a splash of milk, she joyfully obliged. She explained to me that she has been volunteering at the shelter for months, and that she loves it: the shelter residents are amazing, and she enjoys her work. She mentioned that some of them are experiencing tough situations and are a bit harsh on the volunteers, but for the most part they are very grateful to the staff. Understanding that she was knowledgeable on homelessness issues, I asked her what resources are available to the residents who seek mental health aid. She told me that she was not completely sure how accessible it was, but that she knew that a licensed therapist would come in and do volunteer work with some of the residents every once in a while. While I was happy to hear that professional volunteers were benefiting the residents, studies have shown that public psychotherapists are burdened with a high case load which affects the quality of care (Padgett). Further, the long-term benefits of this work cannot be seen without repeated care and access to housing, which can be difficult when people move in and out of the shelter (Caton 72-87). I wondered how effective this method of volunteer-driven mental health care was in addressing the needs that shelter residents had in accessing reliable mental health care.
In order to better understand this issue from a professional’s perspective, I spoke to clinical social worker and psychotherapist Kristen Clayton who has experience working with homeless clients in emergency care departments and in other facilities. She was able to provide deep insight into the reasoning behind the homelessness crisis and the issues that exist with programs that are targeted towards improving homeless mental health. I asked her what programs she has encountered that are available to the homeless who wanted to seek out mental health care.
“So there are […] family health centers and different subsidized clinics that are meant to provide that mental health treatment to anybody that wants to access it. The problem is that they are very impacted, and you know mental health treatment is voluntary unless you are a danger to self, others or incredibly disabled, but even then, you know it is incredibly difficult to force out-patient treatment. You can force inpatient treatment, but we expect people to follow up.” (Clayton)
She explains that when choosing between factors of immediate survival like food and water, or visiting a mental health clinic, the latter would fall to the lower priority. Since there are rarely checkups from the facilities themselves to the homeless, it is difficult for them to consistently maintain their mental health care. Outreach alone has proven to have limited success in solving long-term mental health issues with the homeless, unless combined with a housing solution (Caton 1-20). Having reliable follow-up care is essential to the longevity of the benefits of mental health treatment and ultimately to the goal of keeping housing-insecure people housed.
There are a few models of mental health case management that have been used to improve the long-term efficacy of social welfare programs targeted at the mentally ill homeless. One of these is the standard or “broker” case management technique. It has the overall goal of connecting patients with the resources they need and coordinating its implementation. Broker-style case managers typically have a case load of about 35 clients, and their services are time-limited. The results of this case management technique included better housing stability compared to standard community treatment.
Another method is intensive case management, which involves a more comprehensive approach where the case manager, who must have a clinical degree, collaborates with the patient’s physicians, educates their family on their mental ailment, implements crisis intervention if needed, and monitors their progress. Case managers usually have about 15 clients and are less constricted by time. When combined with housing solutions, the results of this method were better overall life satisfaction.
Finally, there is assertive community treatment, which is the best for patients with severe mental illness, and when studied has the highest overall efficacy. As the most service-enriched treatment mechanism, it combines a team of professionals, including a psychiatrist, a nurse, one or more case managers, and sometimes a social worker, forensic specialist, or housing specialist. The team shares 10-15 clients, and the results show that this method produced the highest overall life satisfaction, lower psychiatric symptomatology, and lower rates of homelessness. When studied, the most effective strategy in increasing housing stability resulted from an intervention that began with housing and support and ended with assertive community treatment. In addition, the net cost of implementing assertive community treatment was found to be lower because of the higher success rates and thus lower need for expensive inpatient mental care (Caton 72-87). Even with this proven, highly effective solution available, the public must support funding homeless interventions in order for policymakers to enact it.
In my experience in the field, I found that volunteers and staff treated the homeless with compassion and hospitality. The homeless who came to the shelter for food or accommodation were generally kind and grateful, happy to accept help. However, one experience I had while volunteering was a bit off-putting. At the end of my breakfast shift, a homeless guest who was visiting the shelter to receive a meal began asking me questions about where I was from. I answered a few casually, and he continued to ask more questions about my ethnicity and then invasive questions I was unwilling to answer. I excused myself and told him my shift had ended, and it was time for me to leave. He seemed upset and raised his voice at another volunteer who had agreed that I needed to go home. I quickly exited and walked about a block down the road before noticing that he was following me on his bicycle while yelling absurd statements that clearly reflected his mental instability. This experience led me to wonder how a homeless person like this could receive suitable mental health care. He would most likely not take the initiative to follow up with a mental health professional, and he may even be labeled as hostile or uncooperative and be turned away from care. How can medical professionals address a case like his, and how can policymakers create programs for a group of people like him? I feared that the general population would see someone like him in public, and it would fuel the anti-homeless sentiment that has developed since the advent of modern-day homelessness in the 1980s (Gowan 44). It may even result in support for increased policing of the homeless rather than implementing affordable mental health care programs (Gowan 54). Without considering the societal and systemic factors that led him to act in this manner, it is difficult for people to address his situation with empathy.
Societal perceptions of the homeless are of great importance when it comes to allocating funding for social services and programs aimed at helping this population (Reutter). One of the regular volunteers at the shelter told me that we needed to be very patient and thoughtful with the people we serve. He explained that we were the only people in their lives who abide by their requests and that anyone else they encounter will treat them with disrespect and as if they are unwelcome. From my observations in the field, I found that compassionate treatment of the homeless resulted in a friendly environment that was conducive to their prosperous mental health and development of a better quality of life. This is how all programs regarding the homeless should be treated. The homeless are simply victims of a flaw in our society that marginalizes them and considers them insignificant. When given the opportunity to get back on their feet, they can, and there are programs that have been proven to be very effective in doing this.
The focus on incarceration in homelessness intervention programs is not only ineffective in addressing the issue of housing insecurity and intrinsically fostering systemic violence, but it is also economically inadvisable. In 2015, it was reported that about half of the $100 million budget in Los Angeles County allocated towards homelessness was used for policing. In fact, often police officers were inappropriately sent to calls requiring mental health professionals (Holland). Also, in 2017-2018, California cities spent more than three times as much on policing than on housing and community initiatives (Graves and Hoene). In a model solution, Eugene, Oregon began its CAHOOTS (Crisis Assistance Helping Out on the Streets) project in 1989 which was pioneering in crisis intervention without law enforcement. This program partners a medic and a crisis worker to respond to non-emergency 911 calls. The results were stark as the city had a $2 million budget and saved $14 million in ambulance costs and an estimated $8.5 million in public health. Also, the need for law enforcement lessened. Other cities like Denver and Olympia have also tried similar programs and noticed benefits (Dholakia and Gilbert).
While an affable environment, the Dorothy Day House cannot be a long-term solution to homelessness. The residents are burdened by an increasing cost of living, while their mental health barriers only worsen. With homelessness levels at an all-time high in California, having increased by 7% between 2019 and 2022, the issue of housing insecurity clearly stems from flaws in a system that does not prioritize the health and security of marginalized peoples (Tobias). As an authority over institutions that foster systemic violence against impoverished people, it is the responsibility of the government to address this injustice. Mental health issues are extremely prevalent among the unhoused and perpetuate the problems that they face. Thus, policymakers and medical professionals must work together to develop solutions to make reliable, high-quality mental health care services accessible to the homeless. The ability to do this relies on high structural competency (Padgett) and approval from the public which is made difficult by the social exclusion of the homeless (Pattison and McCarthy). Using data that shows what interventions are most effective and economically feasible, the problem of homelessness and mental health can be addressed.
Sakeena Baxamusa’s “Homelessness and Mental Health Interventions in California” shows how combining direct, individual ethnographic study with deep and careful research can produce a powerful intervention. The essay was written for Prof. Seth Holmes’s Fall 2022 Art of Writing class, “Inequality and the Body: Health, Medicine, Society and Environment.”
Fall 2022 Award Winner
Works Cited
Caton, Carol L. M. The Open Door: Homelessness and Severe Mental Illness in the Era of Community Treatment. New York, NY: Oxford University Press, 2017.
Clayton, Kristen. Personal Interview.
Dholakia, Nazish, and Daniela Gilbert. “What Happens When We Send Mental Health Providers Instead of Police.” Vera Institute of Justice, 2021, https://www.vera.org/news/what-happens-when-we-send-mental-health-providers-instead-of-police.
Gowan, Teresa. Hobos, Hustlers, and Backsliders Homeless in San Francisco. Minneapolis: University of Minnesota Press, 2010. Print.
Graves, Scott, and Chris Hoene. “California Spending on Law Enforcement, the Legal System & Incarceration.” California Budget and Policy Center, 18 Jan. 2022,
Holland, Gale. “L.A. Spends $100 Million a Year on Homelessness, City Report Finds.” Los Angeles Times, Los Angeles Times, 17 Apr. 2015, https://www.latimes.com/local/lanow/la-me-ln-homeless-cao-report-20150416-story.html
Padgett, Deborah K. “Homelessness, housing instability and mental health: making the connections.” BJPsych bulletin vol. 44,5 (2020): 197-201. doi:10.1192/bjb.2020.49 Pattison, Ben, and Lindsey McCarthy. “The Role of Mental Health in Multiple Exclusion
Homelessness.” Social Policy and Society, vol. 21, no. 3, 2022, pp. 405–421., doi:10.1017/S147474642000069X.
Reutter, L. et al. “Public perceptions of the relationship between poverty and health.” Canadian journal of public health = Revue canadienne de sante publique vol. 90,1 (1999): 13-8. doi:10.1007/BF03404091
Streeter, Jialu. “Homelessness in California: Causes and Policy Considerations.” Stanford Institute for Economic Policy Research (SIEPR), May 2022,
Vogel, Nancy. Housing the Mentally Ill and Chronically Homeless : an Effective Solution, but Counties Need Greater Flexibility. Sacramento, CA: Senate Publications & Flags, 2011.